Abstract
OBJECTIVE: To determine the extent to which chronic illness and disease severity affect patient satisfaction with their primary care provider in general internal medicine clinics.
DESIGN: Cross-sectional mailed questionnaire study.
SETTING: Primary care clinics at 7 Veterans Affairs medical centers.
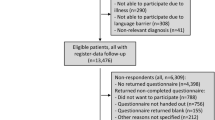
PATIENTS/PARTICIPANTS: Of 62,487 patients participating in the Ambulatory Care Quality Improvement Project, 35,383 (57%) returned an initial screening questionnaire and were subsequently sent a satisfaction questionnaire. Patients (N=21,689; 61%) who returned the Seattle Outpatient Satisfaction Survey (SOSQ) were included in the final analysis, representing 34% of the original sample.
MEASUREMENTS AND MAIN RESULTS: The organizational score of the SOSQ measures satisfaction with health care services in the internal medicine clinic, and the humanistic scale measures patient satisfaction with the communication skills and humanistic qualities of the primary care physician. For ischemic heart disease (IHD), chronic obstructive pulmonary disease (COPD), and diabetes, patient ability to cope with their disease was more strongly associated with patient satisfaction than disease severity. Among IHD patients, improvement in ability to cope emotionally with their angina was associated with higher SOSQ organizational sores (standardized β=0.18; P<.001) but self-reported physical limitation due to angina was not (β=0.01; P=.65). Similarly, in COPD, improved ability to cope with dyspnea was associated with greater organizational scores (β=0.11; P<.001) but physical function was not (β=−0.03; P=.27). For diabetes, increased education was associated with improved organizational scores (β=0.31; P<.001) but improvement in symptom burden was not (β=0.03; P=.14). Similar results were seen with prediction of SOSQ humanistic scores.
CONCLUSIONS: Patient education and ability to cope with chronic conditions are more strongly associated with satisfaction with their primary care provider than disease severity. Further improvements in patient education and self-management may lead to improved satisfaction and quality of care.
Similar content being viewed by others
References
Rosenthal GE, Shannon SE. The use of patient perceptions in the evaluation of health-care delivery systems. Med Care. 1997;35:NS58-NS68.
Davies AR, Ware JE Jr. Involving consumers in quality of care assessment. Health Aff (Millwood). 1988;7:33–48.
Rubin HR, Gandek B, Rogers WH, Kosinski M, McHorney CA, Ware JE Jr. Patients’ ratings of outpatient visits in different practice settings. Results from the Medical Outcomes Study. JAMA. 1993;270:835–40.
Kerr EA, Hays RD, Mitchinson A, Lee M, Siu AL. The influence of gatekeeping and utilization review on patient satisfaction. J Gen Intern Med. 1999;14:287–96.
Hall JA, Dornan MC. What patients like about their medical care and how often they are asked: a meta-analysis of the satisfaction literature. Soc Sci Med. 1988;27:935–9.
Hall JA, Irish JT, Roter DL, Ehrlich CM, Miller LH. Satisfaction, gender, and communication in medical visits. Med Care. 1994;32:1216–31.
Hjortdahl P, Laerum E. Continuity of care in general practice: effect on patient satisfaction. BMJ. 1992;304:1287–90.
Schauffler HH, Rodriguez T. Availability and utilization of health promotion programs and satisfaction with health plan. Med Care. 1994;32:1182–96.
Covinsky KE, Rosenthal GE, Chren MM, et al. The relation between health status changes and patient satisfaction in older hospitalized medical patients. J Gen Intern Med. 1998;13:223–9.
Bidaut-Russell M, Gabriel SE, Scott GG, Zinsmeister AR, Luthra HS, Yawn B. Determinants of patient satisfaction in chronic illness. Arthritis Rheum. 2002;47:494–500.
Hall JA, Feldstein M, Fretwell MD, Rowe JW, Epstein AM. Older patients’ health status and satisfaction with medical care in an HMO population. Med Care. 1990;28:261–70.
Hall JA, Milburn MA, Epstein AM. A causal model of health status and satisfaction with medical care. Med Care. 1993;31:84–94.
Kazis LE, Ren XS, Lee A, et al. Health status in VA patients: results from the Veterans Health Study. Am J Med Qual. 1999;14:28–38.
Xuan J, Kirchdoerfer LJ, Boyer JG, Norwood GJ. Effects of comorbidity on health-related quality-of-life scores: an analysis of clinical trial data. Clin Ther. 1999;21:383–403.
Beinart SC, Sales AE, Spertus JA, Plomondon ME, Every NR, Rumsfeld JS. Impact of angina burden and other factors on treatment satisfaction after acute coronary syndromes. Am Heart J. 2003;146:646–52.
Koning CJ, Maille AR, Stevens I, Dekker FW. Patients’ opinions respiratory care: do doctors fulfill their needs? J Asthma. 1995;32:355–63.
Gross R, Tabenkin H, Porath A, et al. The relationship between primary care physicians’ adherence to guidelines for the treatment of diabetes and patient satisfaction: findings from a pilot study. Fam Pract. 2003;20:563–9.
Redekop WK, Koopmanschap MA, Stolk RP, Rutten GE, Wolffenbuttel BH, Niessen LW. Health-related quality of life and treatment satisfaction in Dutch patients with type 2 diabetes. Diabetes Care. 2002;25:458–63.
Joos SK, Hickam DH, Borders LM. Patients’ desires and satisfaction in general medicine clinics. Public Health Rep. 1993;108:751–9.
Fihn SD, McDonell MB, Diehr P, et al. Effects of sustained audit/feedback on self-reported health status of primary care patients. Am J Med. 2004;116:241–8.
Ware JE Jr, Gandek B. Overview of the SF-36 Health Survey and the International Quality of Life Assessment (IQOLA) Project. J Clin Epidemiol. 1998;51:903–12.
Fan V, Burman M, McDonell M, Fihn S. Continuity of care and other determinants of patient satisfaction with primary care. J Gen Intern Med, doi: 10.1111/j.1525-1497.2005.40135.x.
Webster G. Final Report on the Patient Satisfaction Questionnaire Project. Philadelphia, PA: American Board of Internal Medicine Committee on Evaluation of Clinical Competence; 1989.
Stump TE, Dexter PR, Tierney WM, Wolinsky FD. Measuring patient satisfaction with physicians among older and diseased adults in a primary care municipal outpatient setting. An examination of three instruments. Med Care. 1995;33:958–72.
Harris LE, Swindle RW, Mungai SM, Weinberger M, Tierney WM. Measuring patient satisfaction for quality improvement. Med Care. 1999;37:1207–13.
Davies A, Ware J. GHAA’s Consumer Satisfaction Survey and User’s Manual. 2nd ed. Washington, DC: Group Health Association of America; 1991.
Jatulis DE, Bundek NI, Legorreta AP. Identifying predictors of satisfaction with access to medical care and quality of care. Ann J Med Qual. 1997;12:11–8.
Tu SP, McDonell MB, Spertus JA, Steele BG, Fihn SD. A new self-administered questionnaire to monitor health-related quality of life in patients with COPD. Ambulatory Care Quality Improvement Project (ACQUIP) Investigators. Chest. 1997;112:614–22.
Spertus JA, McDonell M, Woodman CL, Fihn SD. Association between depression and worse disease-specific functional status in outpatients with coronary artery disease. Am Heart J. 2000;140:105–10.
Spertus JA, Winder JA, Dewhurst TA, et al. Development and evaluation of the Seattle Angina Questionnaire: a new functional status measure for coronary artery disease. J Am Coll Cardiol. 1995;25:333–41.
Reiber GE, McDonell MB, Schleyer AM, Fihn SD, Reda DJ. A comprehensive system for quality improvement in ambulatory care: assessing the quality of diabetes care. Patient Educ Couns. 1995;26:337–41.
Efron B. Comparing non-nested linear models. J Am Stat Assoc. 1984;79:791–803.
Hotelling H. The selection of variates for use in prediction with some comments on the general problem of nuisance parameters. Ann Math Stat. 1940;11:271–88.
Lumley T, Diehr P, Emerson S, Chen L. The importance of the normality assumption in large public health data sets. Annu Rev Public Health. 2002;23:151–69.
Kleinbaum DG, Kupper LL, Muller KE, Nizam A. Applied Regression Analysis and Other Multivariable Methods. 3rd ed. Pacific Grove, CA: Duxbury Press; 1998.
Jackson JL, Chamberlin J, Kroenke K. Predictors of patient satisfaction. Soc Sci Med. 2001;52:609–20.
Marple RL, Kroenke K, Lucey CR, Wilder J, Lucas CA. Concerns and expectations in patients presenting with physical complaints. Frequency, physician perceptions and actions, and 2-week outcome. Arch Intern Med. 1997;157:1482–8.
Concato J, Feinstein AR. Asking patients what they like: overlooked attributes of patient satisfaction with primary care. Am J Med. 1997;102:399–406.
Jackson JL, Kroenke K. Patient satisfaction and quality of care. Mil Med. 1997;162:273–7.
Hoffman C, Rice D, Sung HY. Persons with chronic conditions. Their prevalence and costs. JAMA. 1996;276:1473–9.
Von Korff M, Gruman J, Schaefer J, Curry SJ, Wagner EH. Collaborative management of chronic illness. Ann Intern Med. 1997;127:1097–102.
Clark NM, Gong M. Management of chronic disease by practitioners and patients: are we teaching the wrong things? BMJ. 2000;320:572–5.
Plomondon ME, Rumsfeld JS, Humble CG, et al. Factors influencing risk-adjusted patient satisfaction after coronary artery bypass grafting. Am J Cardiol. 2003;92:206–8.
Kerr EA, Smith DM, Kaplan SH, Hayward RA. The association between three different measures of health status and satisfaction among patients with diabetes. Med Care Res Rev. 2003;60:158–77.
Piette JD. Satifaction with care among patients with diabetes in two public health care systems. Med Care. 1999;37:538–46.
Anderson LA, Zimmerman MA. Patient and physician perceptions of their relationship and patient satisfaction: a study of chronic disease management. Patient Educ Couns. 1993;20:27–36.
Kazis LE, Miller DR, Clark J, et al. Health-related quality of life in patients served by the Department of Veterans Affairs: results from the Veterans Health Study. Arch Intern Med. 1998;158:626–32.
Author information
Authors and Affiliations
Corresponding author
Additional information
There are no conflicts of disclose, and there are no financial or personal relationships among the authors that would affect the results of this study.
Deceased.
See editorial by Vinicor, p. 483.
The research reported here was supported by the Department of Veterans Affairs, Health Services Research and Development Service grants SDR 96-002, IIR 99-376, RCD 99-319, and RCD 02-170.
The views expressed in this article are those of the authors and do not necessarily represent the views of the Department of Veterans Affairs.
Rights and permissions
About this article
Cite this article
Fan, V.S., Reiber, G.E., Diehr, P. et al. Functional status and patient satisfaction a comparison of ischemic heart disease, obstructive lung disease, and diabetes mellitus. J GEN INTERN MED 20, 452–459 (2005). https://doi.org/10.1111/j.1525-1497.2005.40057.x
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2005.40057.x